Blogs
Blogs
Healthcare facilities generate seven distinct types of waste that require specific handling and disposal methods. These include infectious waste, pathological waste, sharps waste, pharmaceutical waste, chemotherapy waste, radioactive waste, and general non-hazardous waste. Each category has unique identification characteristics and regulatory requirements that affect the waste management practices hospitals must follow to ensure patient safety and environmental protection.
Healthcare waste falls into seven main categories, each requiring different handling protocols and disposal methods. Understanding these classifications is essential for proper waste management practices that hospitals implement to maintain safety standards.
Infectious waste includes any materials contaminated with blood, body fluids, or potentially infectious substances. This category covers blood-soaked bandages, surgical gloves, laboratory cultures, and pathological specimens from patient procedures.
Pathological waste consists of human tissues, organs, body parts, and recognisable human remains from surgeries, autopsies, or medical procedures. This waste requires special handling due to its sensitive nature and potential disease transmission risks.
Sharps waste encompasses all items that can puncture or cut, including needles, scalpels, broken glass, and lancets. These materials pose immediate injury risks and require puncture-resistant containers for safe disposal.
The remaining categories include:
Improper healthcare waste segregation creates serious risks, including infection transmission, environmental contamination, regulatory violations, and substantial financial penalties. Healthcare facilities have legal obligations to protect patients, staff, and the general public from potential hazards.
Patient safety depends on effective waste segregation because contaminated materials can spread infectious diseases throughout healthcare facilities. When different waste types are mixed together, the entire volume must be treated as the most hazardous category, significantly increasing disposal costs.
Staff protection requires clear segregation protocols because healthcare workers handle waste containers daily. Exposure to improperly sorted waste can lead to needlestick injuries, chemical exposure, or infection transmission, affecting employee health and increasing facility liability.
Environmental protection regulations mandate specific treatment methods for each waste category. Mixing pharmaceutical waste with general refuse can contaminate water systems, while improper sharps disposal endangers sanitation workers and community safety.
Regulatory compliance failures can result in substantial fines, operational shutdowns, and legal liability. Healthcare facilities must demonstrate proper waste management practices to maintain operating licences and avoid costly enforcement actions.
Infectious waste identification relies on recognising materials contaminated with blood, body fluids, or potentially infectious substances. Visual cues include visible blood saturation, laboratory culture materials, and items from isolation rooms or infectious disease treatment areas.
Blood-soaked items require classification as infectious waste when saturation is visible or when materials would release liquid blood if compressed. This includes surgical sponges, bandages, and protective equipment from trauma or surgical procedures.
Laboratory waste includes culture dishes, specimen containers, and any materials used to grow or identify microorganisms. Pathology departments generate infectious waste through tissue samples, slide preparations, and contaminated laboratory equipment.
Different healthcare departments produce characteristic infectious waste streams:
Visual identification training helps staff recognise when general waste becomes contaminated and must be reclassified as infectious material requiring special handling protocols.
Sharps waste consists of any medical items that can puncture, cut, or cause injury through penetration. Unlike other medical waste categories, sharps require immediate placement in puncture-resistant containers and cannot be compacted or processed through standard waste treatment methods.
Physical characteristics distinguish sharps from other waste types by their ability to penetrate skin or standard waste bags. This includes needles, scalpel blades, broken glass vials, and any medical instruments with cutting edges or pointed surfaces.
Handling procedures for sharps differ significantly from those for other medical waste because they require immediate containment at the point of use. Staff cannot transport loose sharps or place them in regular waste containers, even temporarily.
Specialised disposal requirements include:
Prevention protocols focus on eliminating needlestick injuries through safety-engineered devices, proper training, and immediate disposal practices that protect healthcare workers from accidental exposure.
Pharmaceutical waste requires specialised handling because medications can contaminate water systems, create environmental hazards, and pose controlled-substance security risks. Different drug categories require specific disposal methods that prevent environmental contamination and drug diversion.
Controlled substances must be witnessed during destruction and documented according to regulatory requirements. Healthcare facilities need secure storage, chain-of-custody procedures, and authorised personnel oversight when disposing of narcotics and other scheduled medications.
Expired medications cannot be disposed of through standard waste streams because they retain their chemical properties and environmental impact. Flushing medications down drains contaminates water treatment systems and harms aquatic ecosystems.
Chemotherapy drugs require particularly careful handling because they remain cytotoxic even when expired or unused. These medications require specialised high-temperature incineration to ensure the complete destruction of carcinogenic compounds.
Environmental protection measures include:
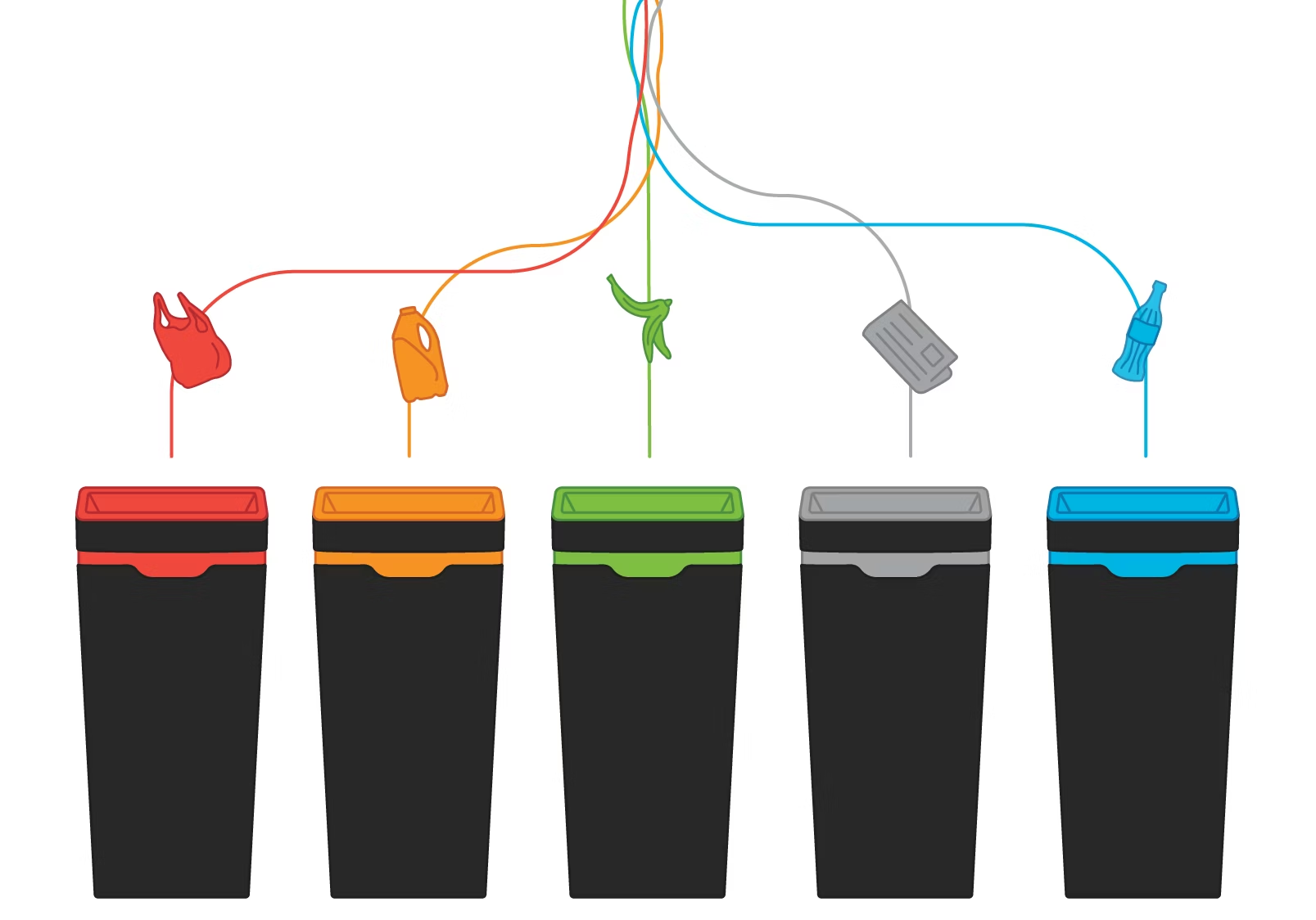
Healthcare waste containers follow international colour-coding systems that visually communicate proper disposal methods and safety requirements. Red containers are used for infectious waste, yellow containers for pathological waste, and blue containers for pharmaceutical waste in many regulatory systems.
Red containers are designated for infectious waste, including blood-soaked materials, laboratory cultures, and contaminated equipment. These containers require biohazard symbols and specific labelling to identify contents for processing at treatment facilities.
Yellow containers are used for pathological waste such as human tissues, organs, and recognisable body parts. Some regions use yellow for all clinical waste, while others reserve it specifically for pathological materials requiring incineration.
Container colour assignments vary by region but generally follow these patterns:
Regulatory standards require facilities to follow local waste management guidelines because colour-coding systems differ between countries and regions. Staff training must address the specific system used at their healthcare facility.
BINBIN provides modular waste separation solutions specifically designed for healthcare facilities' complex waste management requirements. Our systems support proper segregation of all seven waste types while maintaining infection control standards and regulatory compliance.
Our healthcare waste management solutions include:
Healthcare facility managers can experience our solutions through trial placements that demonstrate improved waste segregation efficiency. Contact us to discuss your specific healthcare waste management requirements and develop a customised solution for your facility.
Other articles